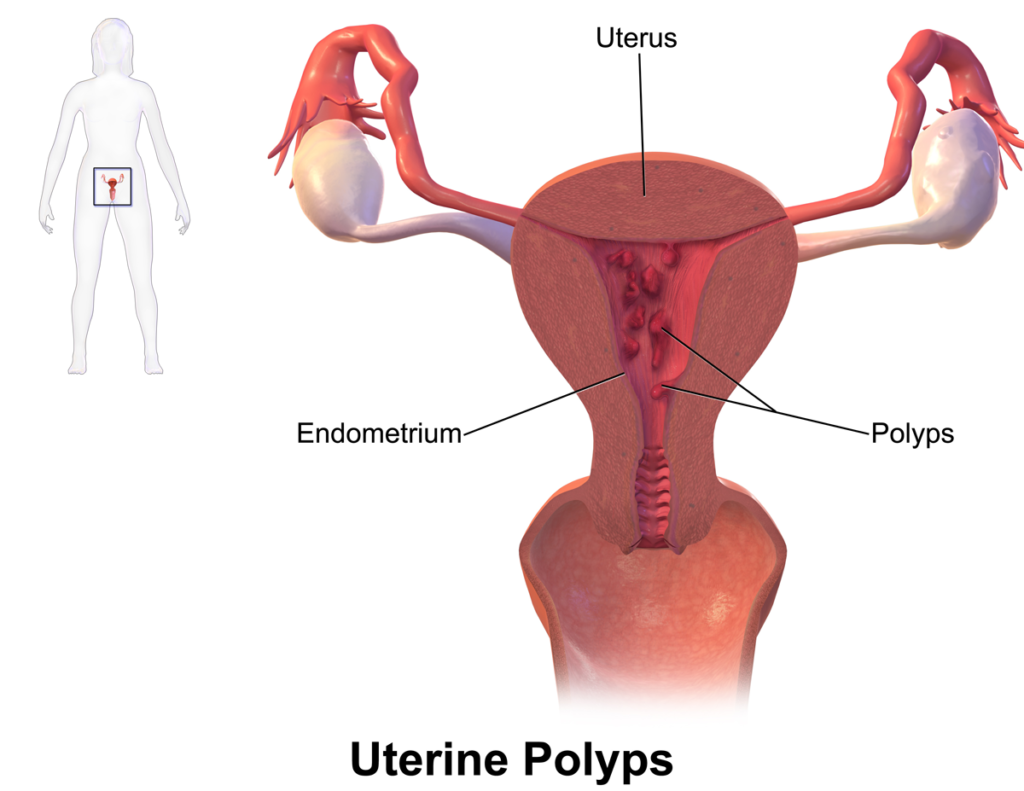
Uterine polyps is a common condition affecting over 1 million people every year in India. They are benign growths attached to uterine lining. Overgrown endometerium cells lead to uterine polyps. They are also called endometrial polyps. It is possible to have more than one polyp. The polyps formed can range from few millimeters to few centimeters. They generally occur within the uterus, but sometimes they may slip into the vagina through the cervix—the lowermost part of the uterus.
The exact cause of uterine polyps is not known. But studies link them to the following:
Estrogen levels: High level of estrogen can cause uterine polyps.
Inflammation: Prolong inflammation of female reproductive system parts like uterus, vagina and cervix.
Risk factors mainly include the factors which increase the estrogen levels.
Related to high estrogen levels:
- Pregnancies & Child bearing years: Estrogen levels are extremely high during pregnancies and child bearing years.
- Pre-menopausal age: After reaching menopause the estrogen levels drop, but just before menopause there is a spike in the levels of estrogen.
- Obesity: Fat cells produce estrogen.
Others:
- High blood pressure.
- Miscarriage
- Herpes
- HPV infection
All most all symptoms of uterine polyps are related to the menstrual cycle.
- Bleeding between menstrual cycles.
- Bleeding after menopause
- Irregular menstrual periods
- Severe menstrual periods
- Infertility
The diagnosis may involve pelvic exam, ultrasound, hysterosonogram and endometrial biopsy.
Pelvic examination: Pelvic examination is a routine screening test wherein the doctor examines various organs such as vulva, ovaries & uterus from outside. The doctor may also use speculum – a device which helps the doctor to view the patient’s cervix and inspect it for abnormalities.
Transvaginal Ultrasound: Ultrasound is an imaging technique which uses ultrasound waves to create an image/video of the internal organs of the patient. In transvaginal ultrasound, the doctor will insert the transducer into the patient’s vagina in order to inspect the uterus with the help of the video/image on screen.
Hysterosonogram: In some cases ultrasound may not be able to show the complications. Hence, to ascertain polyps, the doctor may recommend hysterosonogram. This procedure is similar to ultrasound but in this procedure the doctor also inserts a saline solution into the cavity of the uterus, this helps the doctor to see things which would not be possible with normal ultrasound.
Endometrial Biopsy: Sometimes the doctor may recommend an endometrial biopsy. Here, the doctor will try to obtain sample tissues from the uterine lining for analysis. Most of the patients do not require anesthesia.
Depending on the size of the polyp, the doctor may recommend one of the following treatments.
Watchful waiting: Polyps which are small in size may go away themselves. Medically, there is no reason to treat small polyps unless they are cancerous.
Medication: Medications can provide relief from symptoms, but such relief is likely to be temporary, because in most cases the symptoms are back when the medication is stopped.
Hysteroscopy: Hysteroscopy is a procedure in which the doctor inserts a small, lighted instrument known as the hysteroscope through the patient’s natural orifices. This instrument relays images on the screen, which helps the doctor to inspect the inner organs of the patient and remove the polyps.